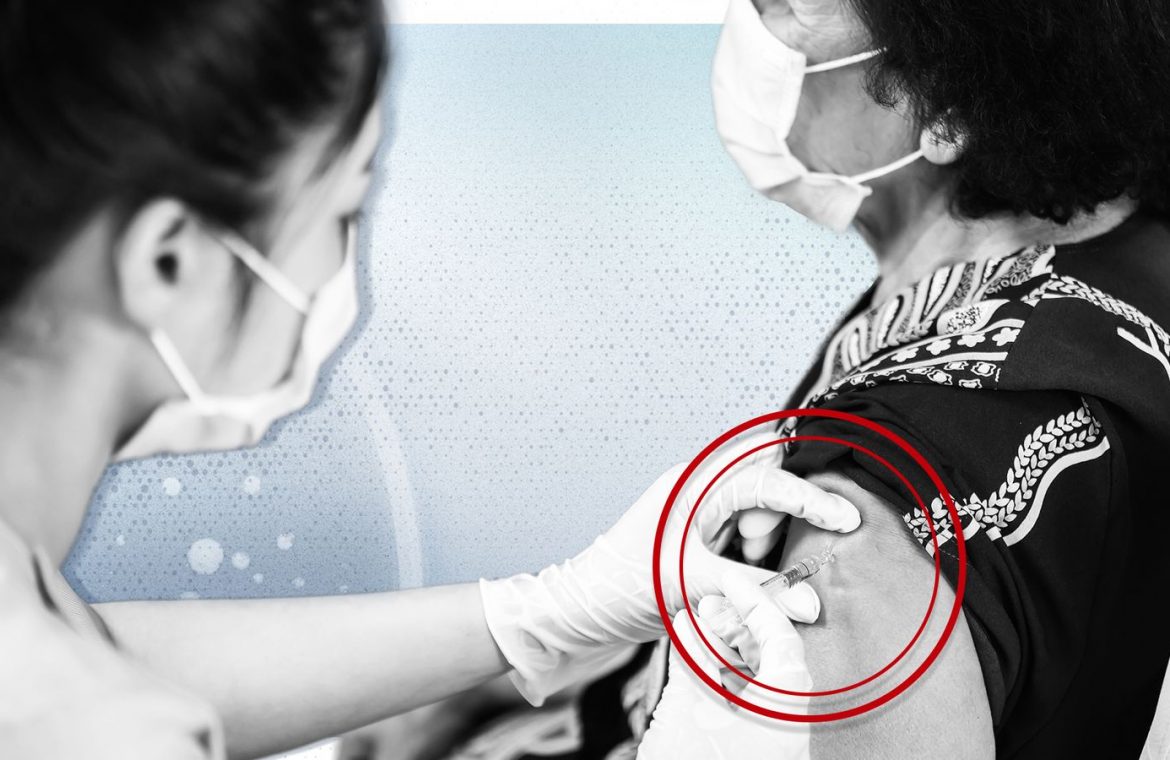
The Pfizer / BioNTech COVID-19 vaccine is being rolled out into GP surgeries starting today.
People will be able to receive the vaccine at more than 100 GP clinics on Mondays and in more surgeries starting Tuesday – a week after the first vaccinations were given approved in hospitals across the UK.
Sky News spoke to the president of the Royal College of General Practitioners (RCGP), Professor Martin Marshall, about how this was happening and who would get the vaccine in the beginning.
Who will get the vaccine and how will they know if they have been selected?
People aged 80 or over will be the first to receive the vaccine in GP surgeries.
Professor Marshall said: “You will receive an invitation if you are in that priority group.
“Please don’t call for surgery to get vaccinated or attend, wait until you are contacted.”
He said that there would be “some flexibility” at the local level to give priority to the most vulnerable groups within that age group, such as some races or people with multiple conditions.
What will be the procedure once a person goes to surgery to get their vaccine?
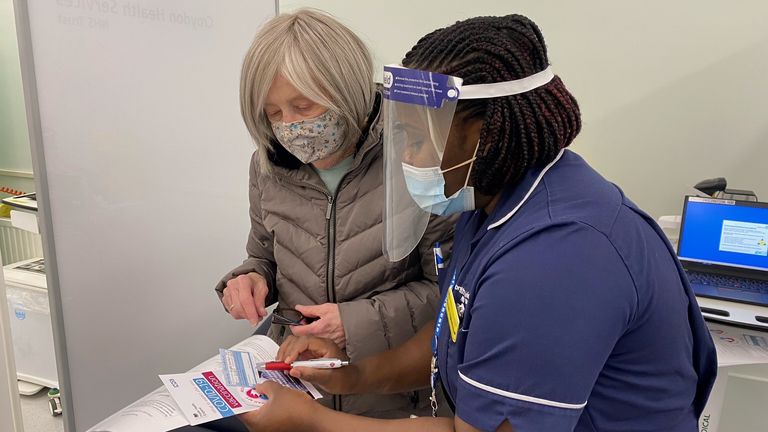
Like getting a flu shot, people will have to arrive at surgery on time and check-in with the receptionist.
Professor Marshall said, “The staff will be in necessary personal protective equipment, and you will be lined up with an appropriate social distance.”
“There will be staff at every stage of the process, who will describe the risks and get the person’s consent.”
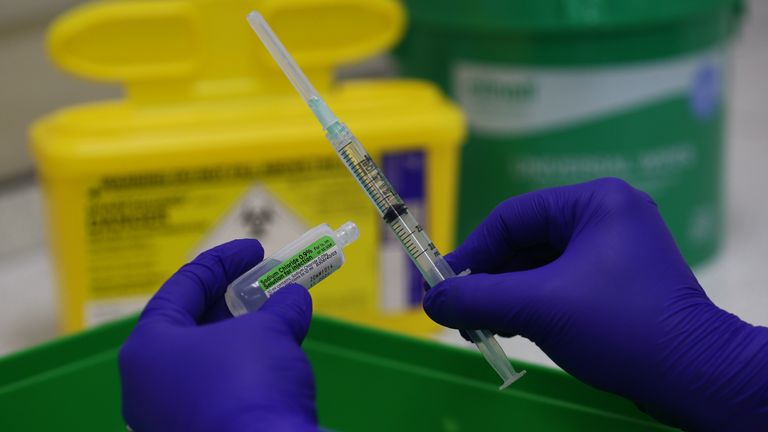
The workers, probably the nurses, will take a vial out of the refrigerator and mix it with a saline solution, ready for use.
After this, the vaccine will be injected into the person’s arm and they will have to wait another part of the surgery for 15 minutes.
What are the risks and is it safe to get vaccinated in a GP clinic?
Since two NHS employees had reactions to the vaccine on the first day of application starting, everyone has to wait 15 minutes before they can leave the surgery.
Anyone with a history of drug or food intolerance should not be invited to get the vaccine.
The risk is low, but if anyone has anaphylaxis, GP surgeries are well equipped to handle it.
Professor Marshall said: “GPs don’t get immediate support from the hospital, but they do have basic life support, oxygen, and peritonism – all the things that will treat anaphylaxis quickly and safely.”
Will all GP surgeries give the vaccine?
No, practices will be chosen by Public Health England (PHE) to become vaccine centers on the understanding that they will remain open for a longer period to ensure that all vaccines they have can be used.
Will the GP’s selected surgeries still provide regular service?
Not every surgery employee will be a part of the vaccination program, but PHE will inform practices chosen to prioritize vaccination.
Patients may be able to get advice over the phone, but Professor Marshall said that if they need “more detailed or urgent care” they can go to a nearby clinic.
It is the busiest time of year for the NHS, and on top of the vaccine, they will continue to offer the flu vaccine and treat the sick.
“Practices will help each other, we are all in this together,” he said.
“The NHS will emerge at its best.”
The vaccine should be stored at -70 ° C, how will GP surgeries handle that?
Professor Marshall explained that vials, which contain five doses each, will be transported from major PHE freezers to hospitals across the UK that have -70 ° C freezers.
“The vaccine can only be transported three times, so once it is placed in the hospital refrigerator, it must be delivered from there to 200-250 individual GPs across the country who have been selected,” he said.
“When they receive a package – 975 vaccines in one box – they’ll put them in the refrigerator in practice, thaw and then have five days to use it all.
“That wouldn’t be perfect, definitely not from day one and you’ll make mistakes, but I hope it isn’t too much.
“We have a strong record of providing mass vaccinations, and I am very confident that general practice can do that well.
“The GP staff are so well trained that I hope the mistakes are minor and we’ll learn very quickly.”
Will the Pfizer vaccine be given to people in care homes?
They will, but because logistics is more difficult than moving it to GP surgeries, the drug regulator, MHRA, is still deciding how best to do it.
Professor Marshall said it wouldn’t be for the first week, but when the startup is approved, the GP or practice nurse will go to the care home and administer the vaccine.
Subscribe to the daily podcast at Apple Podcast, Google Podcast, Spotify, speaker
He said, “The biggest risk in getting them out of centers and into people’s homes is changing the nature of the vaccine or wasting it.”
“We need to be careful before we take a risk.”

“Music specialist. Pop culture trailblazer. Problem solver. Internet advocate.”